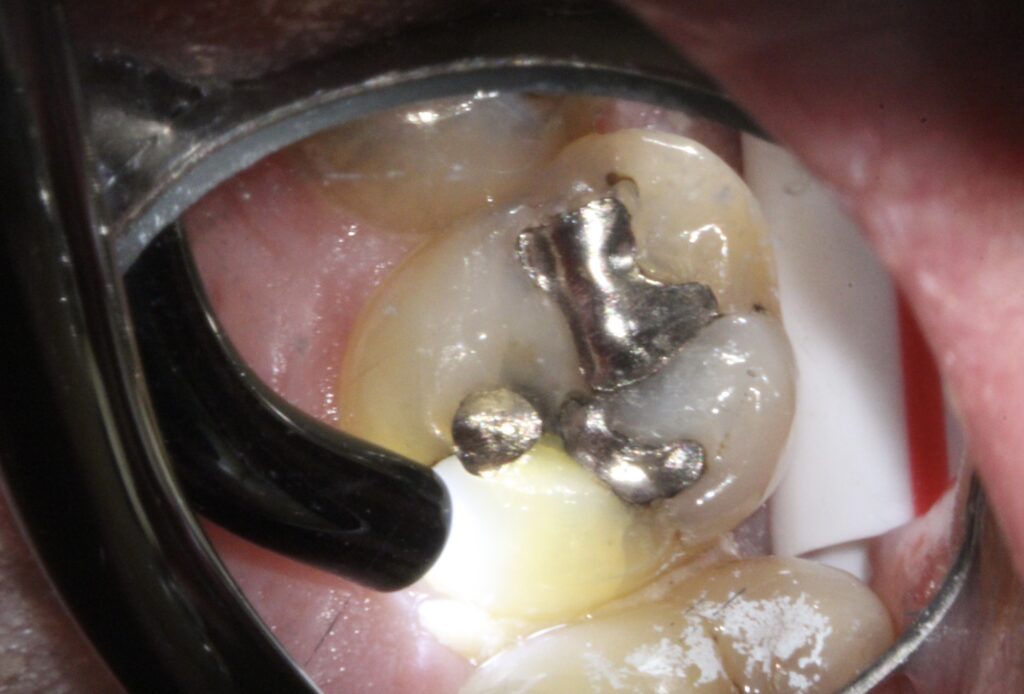
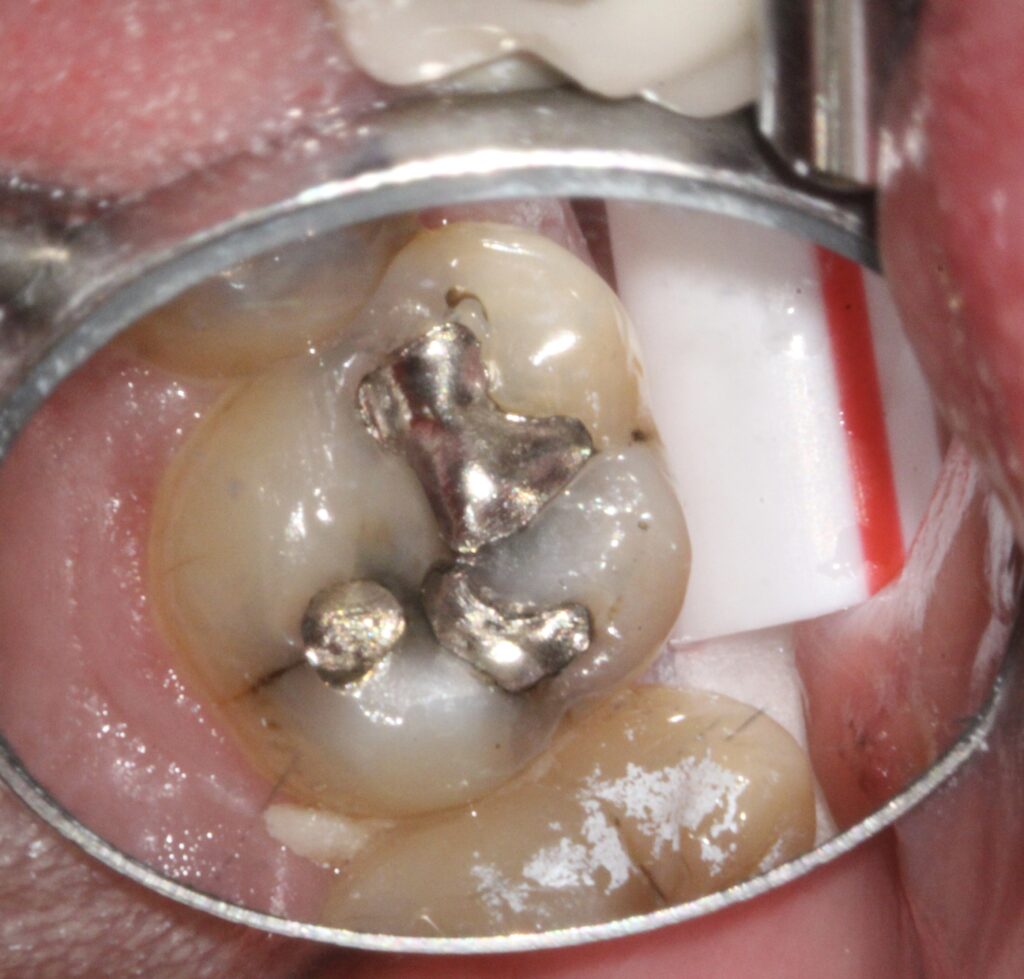
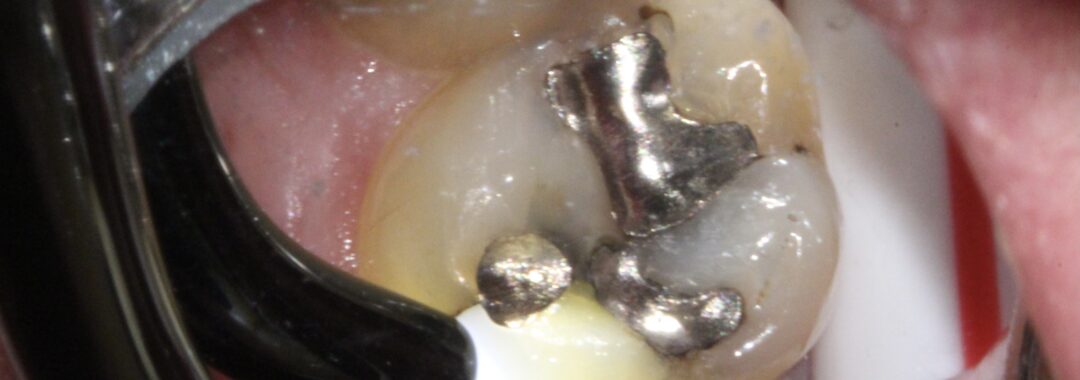
What happens to my tooth when I have to have fillings, crowns, bonding or any other restorations?
To perform dental restorations, the diseased tooth structure and all the old filling material/crowns/etc. have to be removed. Any time a dental drill contacts a tooth, the drill’s rotation causes some tooth trauma. Lots of water and slower drilling speeds are used to minimize trauma to the tooth’s nerve. Unfortunately, there is no alternative to drilling on a tooth to remove old restorations (dental lasers cannot cut old fillings or crowns). Sometimes the actual drilling on the tooth causes postoperative sensitivity and the tooth becomes more sensitive to cold. This is usually temporary but may last for several months.
Teeth that have had a lot of fillings or crowns may also experience more sensitivity after treatment. The difficulty with assessing the health of these teeth, is that we cannot remove them and look at their nerve tissue under a microscope without permanently removing them from patients. Teeth with lots of dental history have had a lot of nerve trauma over their life span. Sometimes these teeth appear to still be healthy and respond well to our nerve tests when in reality there is dead nerve tissue already present and we cannot see it inside the tooth. These teeth may eventually demonstrate signs and symptoms of necrotic nerves and need root canals. We always try to determine nerve health prior to restoring teeth, but sometimes it is just not possible to be accurate due the long dental history of some teeth. That being said, we still only recommend root canals for teeth with apical periodontitis (signs and symptoms of dead nerves) or when clinical judgment dictates a root canal now would be more successful with great access versus later with a new crown present.
Lastly, some teeth which receive dental work have one or more fractures in the tooth enamel which progresses into the dentin. When the enamel structure is disrupted from a fracture, the tooth no longer flexes uniformly. Once the the fracture is covered, the tooth may still experience biting pressure sensitivity. This may mean the new restoration is high and this may be easily adjusted. Alternatively, the tooth structure is flexing in a new and different way with the new restoration. Often, the nerve does not initially respond well to this new movement. That is when you get the “zinger” when you bite just right. If the restoration is correctly adjusted for the bite, this zinger eventually dissipates with time. The time depends on so many factors like the bite force, the wear patterns on the other teeth, the occlusal scheme, the size of the restoration, the age of the patient, etc.
If every tooth and every patient were the same, dentistry would be easy and boring! Hopefully, this helps to explain why some teeth have discomfort after dental work.